The 2025 Dietary Guidelines Just Dropped—and We Need to Talk About It
A Brief History: How Did We Get Here?
Since 1980, the DGA has been issued every five years by the U.S. Departments of Agriculture (USDA) and Health and Human Services (HHS). Over the past 45 years, these guidelines have evolved—sometimes based on science, sometimes based on... other influences. Let's take a quick trip down memory lane:
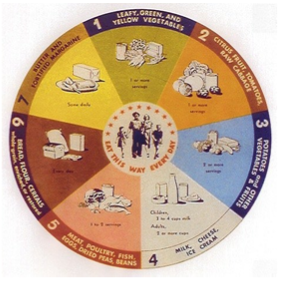

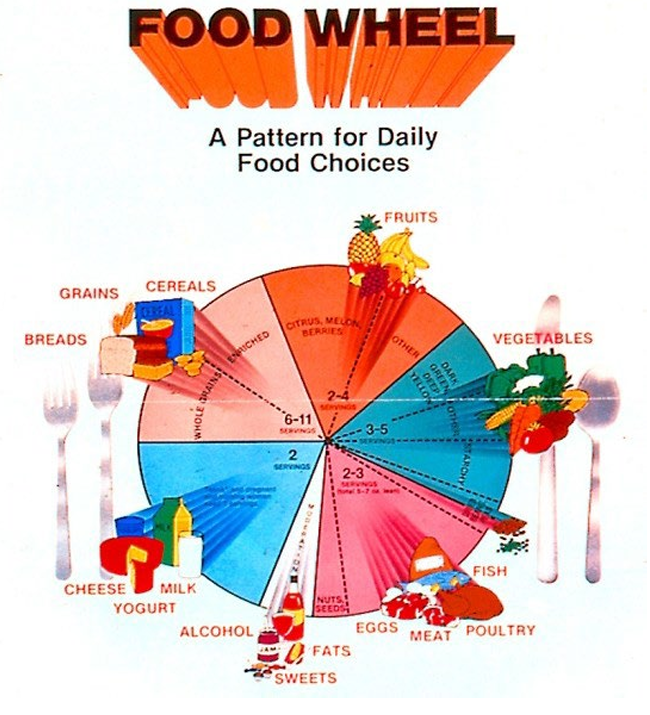
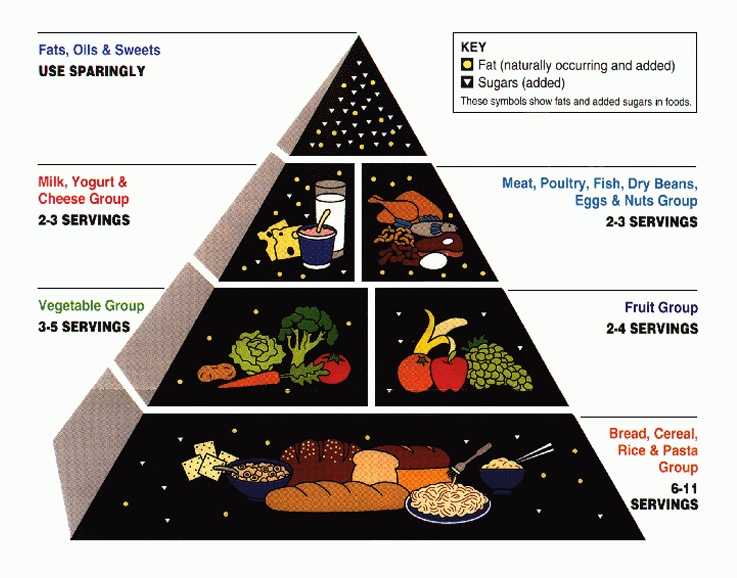



The above graphics are tools that have accompanied the various versions of the Dietary Guidelines for Americans dating back to the 1940s.
1980 Edition: The inaugural DGA featured seven simple guidelines including "eat a variety of foods," "avoid too much fat and cholesterol," and "avoid too much sugar." It was a brief, straightforward document focused on preventing chronic disease.
1985 Edition: Largely similar to 1980 with minor wording changes. This edition introduced the first Dietary Guidelines Advisory Committee (DGAC)—a panel of nine nutrition experts tasked with reviewing scientific literature independently from government agencies.
1990 Edition: A major shift in tone from negative ("avoid") to positive ("choose") wording. This edition emphasized that food could be both enjoyable and healthful, and introduced the first quantitative goals for fat and saturated fat intake. Congress also mandated through the National Nutrition Monitoring and Related Research Act that the DGA must be issued every five years.
1992-2005 Era: The Food Guide Pyramid was introduced in 1992, emphasizing grains as the foundation (6-11 servings daily) with decreasing portions of vegetables, fruits, dairy, and meat/beans. By 2000, the pyramid was refined to emphasize whole grains over refined grains.
2010 Edition: Enter MyPlate, replacing the pyramid with a simple plate graphic showing proportions: half the plate for fruits and vegetables, with smaller sections for grains and protein. This visual made it easier for Americans to understand portion recommendations.
2015-2020 Edition: For the first time, the DGAC considered environmental sustainability in their recommendations, finding that plant-based diets were better for both health and the environment. This sparked significant controversy.
2020-2025 Edition: A comprehensive 164-page document with detailed appendices, transparent methodology, and extensive scientific references developed by a 20-member independent DGAC over two years.
2025-2030 Edition: And now we're here. A 46-page document that rejected the independent DGAC's scientific report due to biases related to health equity and in favor of a separately commissioned "Scientific Foundation" document. This represents the first time in modern history that the government has dismissed the independent advisory committee's findings.
The pattern? When industry influence is minimized and independent scientists lead, we get evidence-based recommendations. When political and economic interests creep in, we get... well, keep reading.
First, Let's Talk About What Changed (And What Didn't)
The 2020-2025 DGA was a hefty 164-page document complete with detailed appendices, transparent methodology, and extensive scientific references (U.S. Department of Agriculture and U.S. Department of Health and Human Services, 2020). It was developed over two years by an independent Dietary Guidelines Advisory Committee (DGAC)—20 vetted nutrition scientists who reviewed mountains of evidence with no strings attached to industry.
The 2025-2030 version? A slimmed-down 46-page document with a brand new website called RealFood.gov that features an upside-down pyramid graphic prominently displaying steak, butter, and whole milk (U.S. Department of Agriculture and U.S. Department of Health and Human Services, 2026).
“Great branding, questionable science.”
Here's where it gets spicy: The current administration rejected the DGAC's scientific report and commissioned a separate "Scientific Foundation" document written by a group selected through a "federal contracting process." Translation? We don't actually know who wrote it or how transparent the process was. What we do know is that some of the reviewers disclosed financial ties to the beef and dairy industries—you know, the same industries whose products are now front and center in the new pyramid.
The Irony of "Real Food" Graphics
Neither pyramids nor real foods present.
Here's a fascinating detail that deserves its own spotlight: RealFood.gov proudly proclaims "Eat Real Food" as its tagline, but here's what you won't find in the pyramid's visual graphics:
No images of real food (just dated graphic illustrations)
No legumes or beans (except one tiny bowl of rice and beans hidden in the protein section)
No lentils, chickpeas, or split peas
No seeds
No whole grain pasta, quinoa, or barley
Minimal representation of whole grain bread (just one loaf)
What you will find prominently featured:
Multiple cuts of red meat (steak, ground beef)
Full-fat dairy products (whole milk, cheese, butter, full-fat yogurt)
Beef tallow listed as a recommended cooking fat
Ultra-prominent placement of animal proteins
For a website claiming to promote "real food," it's conspicuously missing some of the most nutrient-dense, fiber-rich, evidence-supported foods in the human diet. Legumes alone provide plant protein, fiber, essential minerals, and have been associated with reduced cardiovascular disease risk (American Heart Association, 2021). Yet they're virtually invisible in the visual guidance.
The pyramid shows us exactly one serving of oats in a bowl and one loaf of bread to represent the entire "whole grains" category, while animal products get a stunning visual showcase with multiple examples. This isn't just poor graphic design—it's a value statement about what foods matter most. And spoiler alert: that statement doesn't align with the scientific evidence.
With so many contradictions in the current Dietary Guidelines, we can make a game of it.
The Saturated Fat Contradiction
Let's play a fun game I like to call "Spot the Contradiction."
The DGA says: Keep saturated fat below 10% of your total daily calories (for a 2,000-calorie diet, that's about 22 grams) (U.S. Department of Agriculture and U.S. Department of Health and Human Services, 2026).
Also, the DGA: Eat full-fat dairy, steak, butter, and beef tallow as your primary protein and fat sources!
Let's do some quick math, shall we? According to the DGA's own daily serving recommendations
1 cup of whole milk = 5g saturated fat
¾ cup full-fat Greek yogurt = 6g saturated fat
1 oz cheddar cheese = 6g saturated fat
Running total: 17g saturated fat
Now add just ONE tablespoon of butter (7g) or beef tallow (6g)—cooking fats they explicitly recommend—and you're already over the 22g limit. And that's before you've eaten the steak prominently featured in the pyramid, had a snack, or even considered the rest of your meals.
The cognitive dissonance is chef's kiss.
Meanwhile, the scientific evidence is crystal clear: The DGAC scientific review found strong evidence that lower saturated fat intake decreases the risk of cardiovascular disease in adults (Harvard T.H. Chan School of Public Health, 2026). Dr. Frank Hu, professor of nutrition and epidemiology at Harvard, noted that "the mixed messages surrounding saturated-fat-rich foods such as red meat, butter, and beef tallow may lead to confusion and potentially higher intake of saturated fat and increased LDL cholesterol and cardiovascular risk" (Harvard T.H. Chan School of Public Health, 2026).
Yet the new pyramid gives equal visual weight to butter and olive oil, as if they're nutritionally interchangeable. Spoiler: they're not.
Contradiction Bingo Night ahead!
The Sodium Sleight of Hand
Here's another fun contradiction for your bingo card:
The DGA says: Limit sodium to 2,300 mg per day (U.S. Department of Agriculture and U.S. Department of Health and Human Services, 2026).
Also, the DGA: Add salt to your meat for flavoring instead of sugar or simple carbohydrates!
If you're adding salt to every meal as suggested, hitting that 2,300 mg target becomes nearly impossible—especially when you consider that whole milk, cheese, and many other foods in the pyramid already contain significant sodium.
The 2021 American Heart Association scientific statement on dietary guidance for cardiovascular health clearly recommends minimizing intake of processed foods and foods prepared with salt to improve cardiovascular health (American Heart Association, 2021). So why are we being told to season everything with salt while simultaneously keeping sodium intake low? Make it make sense.
What Happened to Plant-Based Foods?
If you squint really hard at the new pyramid, you can find whole grains. They're there—somewhere between the giant steak and the butter. The pyramid suggests 2-4 servings per day of whole grains, which is technically fine, but their visual representation is... minimal at best. Where are the actual grains? Quinoa, farro, oats, etc. This used to be the issue with the original pyramid.
Here's what science actually tells us about plant-based foods:
Nuts and Seeds: A comprehensive umbrella review analyzing 89 articles found that an intake of 28g per day of nuts compared with not eating nuts was associated with a 21% reduction in cardiovascular disease risk (including coronary heart disease incidence and mortality, atrial fibrillation, and stroke mortality), an 11% reduction in cancer deaths, and a 22% reduction in all-cause mortality (Guasch-Ferré et al., 2023). A systematic review and meta-analysis found that consumption of total nuts and seeds is associated with lower risk of cardiovascular disease and coronary heart disease in a dose-dependent manner (Bärebring et al., 2023). These aren't just "healthy fats"—they're disease-fighting powerhouses.
Legumes: The 2021 American Heart Association scientific statement notes that a systematic review comparing high and low intake of legumes concluded that higher intake was associated with lower cardiovascular disease risk (American Heart Association, 2021). Replacing one serving per day of total red meat with nuts was associated with lower risk of coronary heart disease and stroke in the Health Professionals Follow-up Study and Nurses' Health Study, as well as lower risk of cardiovascular disease mortality and type 2 diabetes in multiple large cohort studies (Ros & Hu, 2013). Legumes provide substantial fiber and plant-based protein without the baggage of saturated fat.
Whole Grains: A systematic review and dose-response meta-analysis of prospective studies found that high whole grain intake was associated with reduced risk of coronary heart disease, cardiovascular disease, total cancer, and all-cause mortality, with reductions in risk observed up to an intake of 210-225g per day (seven to seven and a half servings)—nearly double what the new pyramid recommends (Aune et al., 2016). Research published in Circulation found that increased consumption of seeds, including whole grains, nuts, and legumes, is associated with lower risk of cardiovascular disease and type 2 diabetes or a significant reduction in cardiovascular disease risk factors such as serum cholesterol or blood pressure (Ros & Hu, 2013).
But instead of highlighting these evidence-based foods, the DGA gives us a pyramid where red meat and full-fat dairy dominate the visual landscape. It's like they read the research and said, "Nah, beef lobby says otherwise."
The "Essential Fatty Acids" Gaffe
Oh, this one's my favorite. The guidelines suggest prioritizing healthy fats that provide "essential fatty acids" and then list examples: olive oil, butter, and beef tallow (U.S. Department of Agriculture and U.S. Department of Health and Human Services, 2026).
Here's the problem: Butter and beef tallow contain negligible amounts of essential fatty acids (omega-3 and omega-6). They're primarily saturated fat. Olive oil is great, but it's rich in monounsaturated fat (oleic acid), not essential fatty acids.
Dr. Frank Hu from Harvard explained: "Olive oil contains mostly oleic acid, but relatively small amounts of essential fatty acids such as alpha-linolenic acid and linoleic acid compared with other oils that are rich sources of these fatty acids, such as soybean oil and canola oil. Importantly, all these plant oils have been shown to lower LDL cholesterol and cardiovascular risk compared with animal fats such as butter or tropical fats such as coconut oil and palm oil" (Harvard T.H. Chan School of Public Health, 2026).
Want actual sources of essential fatty acids? Soybean oil, canola oil, walnuts, and fatty fish are excellent sources and have been shown to lower LDL cholesterol and reduce cardiovascular risk compared to animal fats like butter.
This isn't a matter of interpretation—it's a factual error. Stanford Medicine's nutrition research group noted that "the guidelines suggest prioritizing healthy fats that provide essential fatty acids, yet the examples provided - olive oil, butter, and beef tallow - contain negligible amounts of the two types of essential fats" and called these "simple factual errors" that "call into question the adequacy of the expert review of the new guidelines" (Stanford Medicine, 2026).
RealFood.gov: A Marketing Masterclass
Let's talk about the website design because, honey, it's something. RealFood.gov features black-and-white bold font, an inverted pyramid design, and messaging that reads more like a wellness influencer's Instagram than official government guidance.
The tagline? "Eat Real Food." Now, this is interesting. This couldn't possibly be targeting plant-based alternatives and food products, could it? I'm sure the dairy and beef industries haven't been affected at all by these "non-real" foods, and there's absolutely no political influence occurring whatsoever. (Insert sarcastic laugh here.)
But let's be real for a moment: "real foods" or "whole foods" have been the focus of the DGA for decades. The 2020-2025 guidelines emphasized "nutrient-dense foods and beverages" and recommended limiting "foods and beverages higher in added sugars, saturated fat, and sodium." The 2015-2020 edition promoted "healthy eating patterns" with "a variety of vegetables from all of the subgroups" and "whole fruits." The 2010 edition introduced MyPlate with a clear emphasis on whole grains, fruits, and vegetables. This isn't new.
Unless you don't think that soymilk is "real." Or that a black bean burger isn't "real food." Because that's where this rhetoric gets dangerous—it creates an arbitrary hierarchy that conveniently aligns with certain industries' interests while dismissing perfectly nutritious, minimally processed plant-based foods that have been consumed for centuries (hello, tofu in Asia since 200 BCE).
The fear-mongering implicit in this "real food" branding insinuates that previous guidelines haven't been transparent or evidence-based, which is demonstrably false. What's actually changed isn't a commitment to whole foods—it's which whole foods get the spotlight, and which ones get relegated to the shadows.
The pyramid is visually simple—I'll give them that. But it prioritizes aesthetics over accuracy. The largest visual section features protein, dairy, and healthy fats, dominated by images of steak, salmon, whole milk, cheese, butter, eggs, and nuts. The vegetables and fruits section is appropriately sized, but whole grains are practically an afterthought. Forget about legumes, nuts, and seeds.
Compare this to the evidence-based Healthy Eating Plate from Harvard T.H. Chan School of Public Health, which gives vegetables and fruits half the plate, whole grains a quarter, and healthy proteins a quarter—with an emphasis on plant proteins. That's what science actually supports.
Where Are the Professional Organizations on This?
Spoiler: Not happy.
The Academy of Nutrition and Dietetics expressed concerns about the departure from established processes and the lack of transparency in the development of the new Guidelines.
The American Society for Nutrition released a statement on January 9, 2026, saying "the decision to introduce a separate Scientific Foundation for the Dietary Guidelines for Americans report instead of the Scientific Report of the 2025 Dietary Guidelines Advisory Committee (DGAC) represents a major departure from long-standing DGA evidence review processes. There is a lack of transparency regarding the methods, approaches, and objectives of the newly introduced scientific reviews and the timeframe in which they were completed. This process diverges from gold-standard National Academies of Sciences-recommended steps for building public and other stakeholders' trust in the guidelines" (American Society for Nutrition, 2026).
ASN also noted that "the departure from the established scientific review process for the Guidelines risks undermining confidence in both the recommendations and the science supporting them, which may contribute to public confusion regarding nutrition guidance. In addition, oversimplification of the Guidelines in ways that introduce contradictory messaging is likely to further confuse consumers" (American Society for Nutrition, 2026).
Harvard T.H. Chan School of Public Health noted that "there appear to be several contradictions within the DGAs and between the DGAs and the new pyramid. The mixed messages surrounding saturated-fat-rich foods such as red meat, butter, and beef tallow may lead to confusion and potentially higher intake of saturated fat and increased LDL cholesterol and cardiovascular risk" (Harvard T.H. Chan School of Public Health, 2026).
Stanford Medicine's Nutrition Studies Research Group pointed out that the guidelines "introduce vague terminology that offers inadequate practical guidance for schools, institutions, and policymakers" and contain "simple factual errors" including the misidentification of olive oil, butter, and beef tallow as sources of essential fatty acids, which "call into question the adequacy of the expert review of the new guidelines" (Stanford Medicine, 2026).
Stanford also highlighted issues with equity and process, noting: "While the 20 members of the DGAC were criticized by the current administration regarding conflicts of interest, the members of the newly assembled committee tasked with preparing the updated guidelines reveal even clearer alignment with the interests of Big Meat, Big Dairy, and Big Food. Notably, the administration cited the DGAC's consideration in its evidence review of a health equity lens as a 'primary concern' and a rationale for dismissing the committee's science-based recommendations. This rationale reinforces structural bias by treating attention to race, culture, and socioeconomic context as illegitimate rather than essential to evidence-based public health guidance" (Stanford Medicine, 2026).
When the nation's leading nutrition science organizations are raising red flags, it's time to pay attention.
The Due Process Problem
Let's compare the development process:
2020-2025 DGA:
20 independent scientists vetted through extensive background checks
Two years of evidence review
Public comment periods
Livestreamed committee meetings
164-page document with full transparency
Based on established scientific methodology (U.S. Department of Agriculture and U.S. Department of Health and Human Services, 2020)
2025-2030 DGA:
DGAC report rejected by current administration
New "Scientific Foundation" by unnamed authors selected via federal contract
Reviewers with disclosed ties to beef and dairy industries
Lack of transparency regarding methods, approaches, objectives, and timeframe
46-page document
Process diverges from gold-standard National Academies recommendations for building public trust (American Society for Nutrition, 2026; Harvard T.H. Chan School of Public Health, 2026)
One of these things is not like the other.
As Dr. Deirdre Tobias, assistant professor in the Department of Nutrition at Harvard Chan School who served on the 2025-2030 Dietary Guidelines Advisory Committee, noted: "As of today, there has not been transparency in who wrote the new DGAs. Although there are documents included in the appendices by named scientists, there is no transparency in the methodology and rigor that was employed, or why certain topics were selected to be relitigated. The reviews themselves, as well as their overall presentation and integration, deviate significantly from the rigorous process that the HHS developed for the DGAs to ensure the evidence base and its committees' conclusions were replicable, unbiased, transparent, and free from non-scientific influences" (Harvard T.H. Chan School of Public Health, 2026).
The Bottom Line
Here's what frustrates me most about these guidelines: They take legitimate nutrition principles—eat more whole foods, reduce processed foods, increase protein intake—and then muddy the waters with contradictory messaging and industry influence.
What science actually supports:
✅ Eat plenty of vegetables and fruits (more than 3 and 2 servings, respectively)
✅ Choose whole grains over refined grains (and eat MORE of them, not less) (Aune et al., 2016)
✅ Include plant-based proteins like legumes, nuts, and seeds regularly (American Heart Association, 2021; Ros & Hu, 2013)
✅ Limit added sugars
✅ Reduce highly processed foods
✅ Prioritize unsaturated fats (from plants, fish, nuts) over saturated fats (American Heart Association, 2021)
✅ Keep sodium reasonable (American Heart Association, 2021)
What the new DGA actually recommends:
❌ Visual emphasis on full-fat dairy, red meat, and butter
❌ Contradictory saturated fat guidance (Harvard T.H. Chan School of Public Health, 2026)
❌ Minimal visual representation of whole grains despite evidence
❌ Confusing sodium messaging
❌ Factual errors about essential fatty acids (Stanford Medicine, 2026)
❌ Unclear guidance on processed foods (Stanford Medicine, 2026)
❌ Nearly invisible representation of legumes, seeds, and diverse whole grains
So What Should You Actually Do?
As a registered dietitian, here's my honest take:
“Don't throw evidence-based nutrition out the window because one set of guidelines missed the mark.”
The research is robust and consistent. Plant-based dietary patterns rich in vegetables, legumes, lean proteins, nuts, seeds and fruits with moderate amounts of whole grains are associated with lower risk of cardiovascular disease and type 2 diabetes (American Heart Association, 2021; Ros & Hu, 2013).
Replacing just one serving per day of total red meat with nuts was associated with lower risk of coronary heart disease, stroke, cardiovascular disease mortality, and type 2 diabetes in multiple large cohort studies including the Health Professionals Follow-up Study, Nurses' Health Study, EPIC-InterAct, and the Women's Health Initiative (Ros & Hu, 2013; Bärebring et al., 2023).
That doesn't mean you can never eat steak or enjoy butter. But it does mean the bulk of your diet should come from plants, with animal products playing a supporting role—not stealing the show.
My Challenge to You
Instead of following a pyramid that contradicts its own recommendations, try this:
Fill half your plate with vegetables and fruits at most meals
Choose whole grains like quinoa, brown rice, oats, and whole grain bread
Include plant proteins like beans, lentils, nuts, and seeds regularly
Enjoy fish and seafood twice per week
Use olive oil as your primary cooking fat
Limit red meat and full-fat dairy to occasional rather than daily consumption
Reduce added sugars and sodium from processed foods
This approach is supported by decades of research, major health organizations worldwide, and—importantly—it won't have you doing mental gymnastics to reconcile contradictory recommendations.
Final Thoughts
Look, I get it. Nutrition is complicated enough without official government guidelines adding to the chaos. But here's the thing: When we follow the money and examine the process, the picture becomes clearer.
“Science hasn't changed. What's changed is who's writing the guidelines and what interests they represent.”
So, my advice? Trust the research, not the inverted pyramid. Trust the experts who don't have financial ties to the industries they're evaluating. And trust your body when you eat more plants and less oversalted, deep fried, sugar-filled food—because that's when most of us feel our best.
Stay nuanced, friends. We're all just trying to eat well and live well in a world that makes it unnecessarily complicated.
References
American Heart Association. (2021). 2021 Dietary Guidance to Improve Cardiovascular Health: A Scientific Statement From the American Heart Association. Circulation, 144(23). https://doi.org/10.1161/cir.0000000000001031
American Society for Nutrition. (2026, January 9). American Society for Nutrition Calls for Strong Science in National Nutrition Guidance. Retrieved from https://nutrition.org/american-society-for-nutrition-calls-for-strong-science-in-national-nutrition-guidance/
Aune, D., Keum, N., Giovannucci, E., Fadnes, L.T., Boffetta, P., Greenwood, D.C., et al. (2016). Whole grain consumption and risk of cardiovascular disease, cancer, and all cause and cause specific mortality: systematic review and dose-response meta-analysis of prospective studies. BMJ, 353:i2716. https://doi.org/10.1136/bmj.i2716
Bärebring, L., Thorisdottir, B., Arnesen, E.K., et al. (2023). Nuts and seeds consumption and risk of cardiovascular disease, type 2 diabetes and their risk factors: a systematic review and meta-analysis. Food & Nutrition Research, 67. https://doi.org/10.29219/fnr.v67.8961
Guasch-Ferré, M., Liu, X., Malik, V.S., et al. (2023). Consumption of Nuts and Seeds and Health Outcomes Including Cardiovascular Disease, Diabetes and Metabolic Disease, Cancer, and Mortality: An Umbrella Review. Advances in Nutrition, 14(4), 726-747. https://doi.org/10.1016/j.advnut.2023.04.003
Harvard T.H. Chan School of Public Health. (2026, January 9). Dietary Guidelines for Americans 2025-2030: Progress on added sugar, protein hype, saturated fat contradictions. The Nutrition Source. Retrieved from https://nutritionsource.hsph.harvard.edu/2026/01/09/dietary-guidelines-for-americans-2025-2030/
Martínez-González, M.A., Gea, A., & Ruiz-Canela, M. (2019). The Mediterranean Diet and Cardiovascular Health: A Critical Review. Circulation Research, 124(5), 779-798.
Ros, E., & Hu, F.B. (2013). Consumption of Plant Seeds and Cardiovascular Health: Epidemiologic and Clinical Trial Evidence. Circulation, 128(5), 553-565. https://doi.org/10.1161/circulationaha.112.001119
Stanford Medicine. (2026). What the 2025-2030 Dietary Guidelines Get Right—and Where They Fall Short. Retrieved from https://med.stanford.edu/nutrition/news/press/2025_2030_Dietary_Guidelines.html
U.S. Department of Agriculture and U.S. Department of Health and Human Services. (2020). Dietary Guidelines for Americans, 2020-2025. 9th Edition. Retrieved from https://www.dietaryguidelines.gov/
U.S. Department of Agriculture and U.S. Department of Health and Human Services. (2026). Dietary Guidelines for Americans, 2025-2030. Retrieved from https://cdn.realfood.gov/DGA.pdf










